I recently attended the national Australian Medical Association (AMA) conference, where the importance of doctors’ health was a major focus.
Our current President, Dr Tony Bartone, spoke of it at length in his opening address, and he reaffirmed the AMA’s support for the updated World Medical Association Physician’s Pledge – the Declaration of Geneva – that now includes the statement:
“I will attend to my own health, wellbeing and abilities in order to provide care of the highest standard.”
Several of the leading lights in the field including Dr Michael Myers, Dr Helen Schultz, Dr Mukesh Haikerwal, Dr Geoffrey Toogood, Dr Jessica Dean and Dr Penny Browne were there too, and it was heart-warming to see these caring, committed people in action and interacting with each other and with the audience.
Dr Myers said it was vital to keep talking about doctors’ health to ensure it remains a high priority on the profession’s agenda.
“In so many respects, we’re still a vocal minority, but I just see that getting louder and louder,” he said.
How strange, that those of us who speak out about doctors’ health are a “vocal minority.”
What is it about medical training that makes us come to think our own health and wellbeing is no longer a priority?
Those of us who go into medicine are no less caring of ourselves than any other young people.
Yet somehow in the process of training to be a doctor, we learn to put others’ needs before our own, to work and work and work no matter how we are feeling, and in some cases to work until we cannot go on any more and burn out, drop out, get sick, or die.
Being brought to a stop
I have been pondering on all this for the last few weeks as I have been resting more than usual, having tripped and fallen and badly broken my left big toe just outside the hotel at the same conference.
I hobbled back inside, made light of it all, and had lunch with my friends with my feet up. I managed to drive myself home (a very long 2 hour drive!) the next day thinking I had just sprained my toe badly, then rested for the rest of the weekend and went to work on Monday as usual. I played down the severity of the fall and my symptoms to my concerned friends and family, so they did not worry so much … and to myself. I was feeling sick and exhausted from the pain, but I just kept playing it down, thinking I had to work. My only concession was to work shorter days, and then come home and rest.
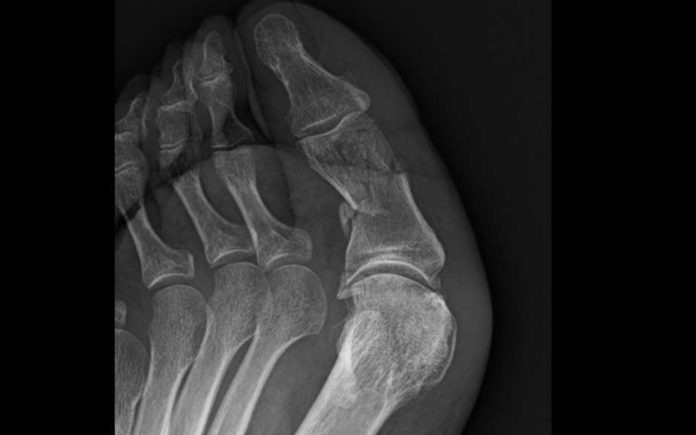
After 11 days of this, my staff insisted I get an X-ray (!) and by this time the swelling had gone down a little and I was becoming more, not less, uncomfortable, and having trouble sleeping at night, so I reluctantly agreed.
When I saw the shattered bone on the X-ray I felt shocked and shattered too … that I had been so willing and able to override what I was actually feeling for the sake of a belief that I just had to keep working.
I did go and see an orthopaedic surgeon (not straight away, but the next day in my lunch break) who laughed at me when I asked him why I did not realise it was broken, and said: because you are a doctor. I felt slightly more reassured and slightly less embarrassed, to know that he knew it was a cultural problem, and not just a personal one, but I felt sad that we as a profession, including myself, know that we don’t take care of ourselves the way we care for others.
Even then I did not fully comply with suggested treatment and agreed to tape the foot but politely (or was that defiantly?) refused the offer of a supportive moon boot … so I hobbled around for another few days until a friend lovingly but firmly told me to get one.
When I first put my foot in the moon boot, I felt so raw and vulnerable … my toe, which had been cushioned in cashmere and lambswool (I had been wearing my Ugg boots to work and no-one blinked an eye – I love being a country doctor!) was now feeling exposed and cold. For some reason it really brought home to me the fragility of my situation and the disregard of my precious body that I had been in.
Why do we override the knowing of our bodies?
It is not that we don’t know what is going on – we just don’t want to know. We think we have to do – whatever it is – and we just keep soldiering on, no matter how we are feeling. We think that our patients won’t be able to manage without us, that we won’t be able to pay our bills, that our business will suffer … if, like me, you are in solo private practice there is a physical reality to these concerns … we have a host of ‘good’ reasons as to why we need to keep working, but we are doing it at our own expense.
And what quality of care are we delivering in that state? Can we truly care for others if we are exhausted, in pain, feeling sick, have the flu, have cancer, depression, anxiety, burnout, drug and alcohol problems, cynicism … and the list goes on, of the many ways in which we can be ill and suffering.
We need to make doctors’ health a priority, at least equal to that of our patients and indeed all people.
And when I say at least equal, it is because we are role models for our patients. We may say “do this” but that statement has much more power if we are actually doing it for ourselves. If we can make our own health a priority, through role modelling and authentic inspiration and speaking from lived experience, we can have a profound influence on the health and wellbeing of our patients, colleagues, staff, family and friends.
Doctors are supposed to be the accepted authority on health and wellbeing. Let’s start to develop true authority by attending to our own. Without that authentic self-care, we may have great knowledge, but we are not speaking from the lived wisdom of a body that knows and lives what is healthy and supportive for us and what is not.









This is so relevant to all health professionals Anne. It is probably the reason that burnout is so prevalent in the nursing profession.
Agreed, Anne, and is probably relevant to all professionals! The irony is that health professionals seem to be the worst of all at caring for themselves, so what sort of standards are we setting and role models are we being for the rest of the community, given that we have committed to care for them?! Nothing much has to change … just us learning to care for ourselves and those who are in charge of us learning to care for and respect us as people, not just service providers…!
It is heartening to hear that there is a vocal minority bringing focus to this issue. Change in professional culture is slow but it will happen. As with the example of your broken toe, our bodies are on the side of bringing more self-care to medicine.
Very true, Fiona, we can try and ignore the messages our bodies send us to let us know that we are needing to make changes in the way we live, but if we do, the messages just get louder, until we are forced to stop and listen!
I appreciate the gift of these blogs as they help to remove the ‘beliefs’ that if someone is a doctor then they are immune to getting sick and do not experience the many health symptoms suffered by so many of the population. I realise that when a doctor or other reads of this belief they may be shocked but I see so many situations where a doctor is set-up on a pedestal and their human-ness is over-looked and disregarded. When I have been treated by a doctor who is connected to their own health and caring of their own body, I have been exposed to an experience of being deeply cared for and supported. Thank you Anne for sharing your own vulnerability with us
Thank you Christine, I really appreciate you taking the time and care to write … I too seek out doctors who care for themselves and who are willing to be vulnerable and human … I feel much more cared for by people who care for themselves too …